Diving Accident Scenario 2: Diver With Rash
A second diving casualty scenario to test your diving incident management and diver medic knowledge. This scenario concerns a diver with a rash.
Diving Accident Scenario: Diver with Rash
Our next diving accident scenario features a 57 year old diver with 47 logged dives (mix of warm and cold water dives) has completed a 2-dive day of diving in March, out of Plymouth (UK). He has been diving from a hard-boat with a ladder for exiting the water. The diver has been using a tank with a 15L tank with a 3L pony, both filled with air. He has a new dive computer and a new dry-suit.
Dive 1: Maximum depth of 32 metres with a 40 minute bottom time. He completed all mandatory decompression stops as well as a 3 minute safety stop.
This was followed by a 1.5 hour surface interval. Wind speeds averaged 4 knots, gusting a maximum of 7 knots. It was a cold spring day with heavy rain and little cover on the boat.
Dive 2: Maximum depth of 18 metres with a total dive time of 60 minutes. This was a drift dive although he and his buddy did spend significant period of time finning against the current to take photos of marine life. He did not incur any decompression and completed a 3 minute safety stop.
The boat returns to port and our diver stows his kit and removes his dry-suit. He feels tired and on removing his under-suit his buddy notes an unusual rash over his torso pictured below.

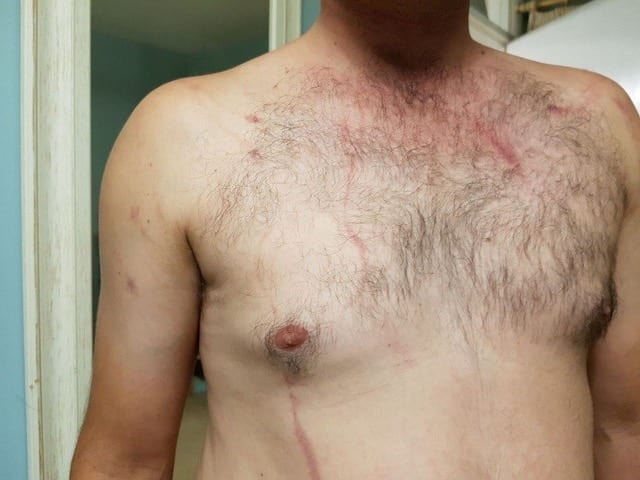
What has happened? What would you do next?
Feedback from Facebook
Originally we posted this diving accident scenario on Facebook, on 25th August 2017. Here are some of the responses received on our Facebook page, which might help (or hinder!) your thoughts:
“Diver well, no issues with dives so I am going to suit squeeze monitor and have more faith in buoyancy control on next dive to use suit.” [KC]
“It looks like squeeze, but better safe than sorry so… Mark the outside of the rash with a pen to be able to easily monitor growth or reduction in size. Administer O2 and monitor. Call either the navy diving doctor, DDRC or 999 and ask for the coastguard.” [CL]
“This does look like squeeze related contusions. Tiredness may be consequence of heavy work during dive, but has been anecdotally linked to sub-clinical DCI. It is clearly stated that deco was completed and fully mitigated nitrogen loss and an additional margin was included. These points do not address the divers general fitness, condition or any underlying health concerns. Monitor closely for 24 hours. O2 treatment won’t help bruising but it will not cause any harm. If there is a DCI element, O2 will be of benefit. Rash likely will worsen as bruising develops over 24 hours. Aid monitoring by marking off bruises with a sharpie or similar and watch for spread. If rash spreads, becomes itchy, or neurological symptoms develop, evac immediately.” [DG]
“Sit or get someone to sit with the diver to monitor, administer O2 and give fluids. Monitor buddy and call DDRC saying a diver has possible signs of decompression illness. If a marker pen is available, mark around the rash to see if increases with time.” [SCB]
“Hopefully suit squeeze however mark rash and photo it. Probably caused by wearing suit for hours zipped up due to weather / exposure. Check skin top of chest and neck feel for crackly emphasema, if present sit, O2 and contact DDRC. Monitor breathing and neuro and rash for improvement.” [ST]
“Old guy with not too much training. Underwater efforts. Both dives are at parameters limits. Use your O2 kit and take him to chamber.” [AA]
“I believe it is skin bend due to lack of water prior to the dives, drinking water that is. And not possibly building his dive up prior to 2 days of constant diving. I would brief hundred percent O2 for at least 20 minutes drink plenty of water and definitely not dive for at least 48 hours. Within the first 24 hours see if increase or decrease or if in doubt always telephone DDRC for advice. Or it could be a simple saying not to equalise the pressure in a suit but I don’t think so. ” [EH]
“Membrane or neoprene suit? Monitor, check motor skills, inform DDRC Healthcare and ask for advice” [BT]
“Suit squeeze! But would recommend O2 and monitor diver. You can never be too safe” [NA]
“Looks like squeeze bruises I get from my suit if I don’t inflate it enough” [DT]
“Looks like pinch marks from the dry suit or an allergic reaction? Burst blood vessels maybe?” [AM]
The Scenario Continues…
This diver has developed signs and symptoms after diving. He has been conducting dives with a high nitrogen exposure requiring decompression, coupled with exerting himself both underwater and on exiting the water via a ladder. Due to the weather conditions he has remained zipped into his drysuit for the day and as a result has been consuming less fluid in an attempt to reduce his need to urinate. This means he is very likely dehydrated. He is using new equipment with a new drysuit and a new computer. These are all risk factors for developing decompression sickness.
Assessment
As with any potential diving incident you should always assess the diver using and ABCDE assessment.
Airway: the diver is talking normally in full sentences, his airway can be considered clear.
Breathing: hi is not complaining of any chest pain or shortness of breath. His respiratory rate is 12 breaths per minute and he is not requiring excessive effort or taking shallow breaths.
Circulation: the diver is talking in full sentences, at his wrist you are able to feel a pulse at 70 beats per minute. Looking at his fingertips however they do appear blue.
Disability: the diver feels tired, but he is alert on the AVPU scale (Alert, responding to Voice, Pain, or Unresponsive). You complete a DDRC 5 minute neurological examination that demonstrates no abnormalities.
Exposure: in the warmth of the dive shop the diver removes his undersuit. It reveals a linear rash pattern, confined to his torso. It is painless but slightly itchy.
What Should You Do?
Until proven otherwise, it should be assumed that the diver in this diving accident scenario is suffering from decompression illness (DCI). He should be placed on oxygen, either via a high flow non-rebreather mask, or as he is alert and talking it would be appropriate to administer oxygen via a demand valve regulator.
Oxygen therapy should not be delayed in order to do so, but taking photographs of the diver’s rash and demarcating it with a marker pen will be very useful for the assessing doctor. Rashes can progress or receded rapidly, particularly with the use of oxygen in a skin bend rash (also known as cutis marmarata). Having good pictures greatly assists with diagnosis.
As he is alert and his airway is clear the diver should be given up to 1 litre of fluids (non-alcoholic, non-caffeinated).
Since the diver is currently well, it is appropriate to contact the British Hyperbaric Association (BHA) National Diving Accident Helpline. In England & Wales 07831 151 523. In Scotland 0345 408 6008.
The diver should be monitored continually and any deterioration would prompt the involvement of emergency services via 999.
What is your diagnosis?
Given the risk factors he was asked to attend DDRC Healthcare where he received a full examination. Other than the rash, no other abnormalities were found. The rash was a clearly demarcated, linear rash. When compared to photos taken immediately after noticing the rash, it has neither progressed nor receded with oxygen. As such it was deemed that this was a simple suit squeeze.
He did not need recompression.
A follow up call the subsequent day showed that he remained well and the rash was beginning to fade.
People are often reluctant to contact the BHA as they are concerned that calling for advice always results in recompression, which in turn leads to enforced time off diving. In the first 8 months of 2017 our figures show that only 18% of calls to the BHA National Diving Accident Helpline resulted in a diver attending and being treated in a hyperbaric chamber.
Divers who do ring and just receive telephone advice often find it very reassuring. If you have any concerns after diving, please don’t sit and worry about potential symptoms, just give us a call.